- Home
- Services
- Center for Lung Health
- Interventional Pulmonology
Interventional Pulmonology
At Cabell Huntington Hospital, our interventional pulmonologist Dr. Yousef Shweihat has undergone extensive training to provide patients with the best pulmonary treatment available.

Dr. Yousef Shwiehat
Interventional Pulmonology is a relatively new specialty within the practice of pulmonology and critical care medicine that has dramatically changed the approach to diagnosing and treating pleural (lung) diseases, evaluating pulmonary nodules, diagnosing, staging and treating lung cancer. The scope of this practice concentrates on diseases involving the airways and the pleural cavities (the area surrounding the lungs). In addition to the general practice of pulmonology, a big part of the interventional pulmonary practice concentrates on procedures that require special training that general pulmonologists usually do not acquire during their fellowship. Interventional pulmonologist Dr. Yousef Shweihat is one of the few in the country who underwent extensive training through a special fellowship to acquire experience in this new field.
Procedures offered through our interventional pulmonology program
Combined EBUS and EUS at the same session
These are two procedures that usually require a lung doctor and a GI doctor (gastroenterologist or stomach doctor) to perform. Because Dr. Shweihat is specially trained in both procedures, he can perform them both himself using one small scope. This procedure can be used for:
- Non-invasive pathologic lung cancer staging* Before considering surgery to treat lung cancer, physicians must know if it has spread to the lymph nodes. This staging procedure, which is usually performed on an outpatient basis, replaces a surgical procedure called mediastinoscopy. Many studies have shown equivalent or even better outcomes with this procedure than mediastinoscopy.
- Investigation of enlarged lymph nodes in the chest of any etiology
- Diagnosis of sarcoidosis
- Diagnosis of lymphoma in the chest
Rigid bronchoscopy
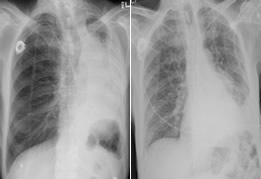 This is an example of X-rays showing the left lung prior to and immediately after the application of rigid bronchoscopy, ablative therapy and airway stenting. Prior to the procedure, the left lung was almost completely collapsed. After the procedure, the left lung is wide open.
This is an example of X-rays showing the left lung prior to and immediately after the application of rigid bronchoscopy, ablative therapy and airway stenting. Prior to the procedure, the left lung was almost completely collapsed. After the procedure, the left lung is wide open.
This is a very old procedure that has been replaced by flexible bronchoscopy. Recently, there has been an increased interest in this procedure in treating airway obstruction (blockage). Patients with obstruction of the airway due to cancer, a foreign body or a benign disease might benefit from such a procedure. The only way to insert certain types of stents or devices to treat the airways is through the rigid scope, and our center is one of few in the country to offer this procedure.
Airway stenting
Airway stents are similar to coronary (heart) stents. They are usually used if the airways are blocked or collapse easily after treating a blockage. They are used for both benign and malignant disease. Our program is well equipped for placing a variety of available stents.
Ablative therapy
Many modalities are available for removing a tumor or opening airway obstruction. Electrocautery, APC and laser therapy are a few of the most commonly used procedures to achieve airway patency. Our pulmonologist had special training in applying such therapies through flexible and rigid bronchoscopy.
Upper airway and tracheal stenosis
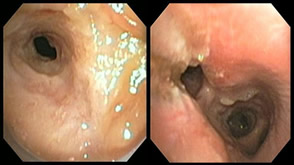
This is an example of a trachea that is stenosed. On the left is the airway before therapy and on the right is the main airway after. Notice that you can see the distal airway (the main carina here) after therapy.
Many diagnoses are benign (non-cancerous), but some may be malignant. The application of ablative therapy through flexible or rigid bronchoscopy is one way to avoid surgery. The endoscopic treatment of these diseases is equivalent if not superior to the complex surgery often recommended to treat these diseases.
Pleural effusion and pneumothorax management
Pleural effusion, the collection of fluids around the lungs, can be caused by many diseases. Often, these diseases are hard to diagnose and treat. Our lung program offers less invasive techniques for diagnosis and treatment that can often replace surgery.
Pleuroscopy
This procedure is much less invasive than the open surgical technique and yields similar results. During a pleuroscopy, a scope is placed in the chest to examine where the fluid collects, take biopsies and seal the space if necessary. A pleuroscopy is typically much better tolerated than the surgical approach, with fewer complications. After the procedure, the patient is expected to be in the hospital for a few days with a chest tube in the side. For selected patients, an indwelling catheter can be placed at time of the procedure.
Indwelling pleural catheters
Often, pleural effusion recurs even after surgical treatment. In some instances patients are not fit enough to undergo surgery or pleuroscopy for treatment. The insertion of a catheter that the patient can use to empty fluids from the chest (whether malignant or not) makes patients more mobile and able to go home. The catheter itself will cause the space where the fluid collects to get sealed in about 70% of patients. If that happens, the tube can be removed easily in the office. This is an outpatient procedure and patients can go home the same day with their care givers.
Chronic hypoxia: Transtracheal oxygen
Many patients need oxygen for their chronic pulmonary diseases. Often, even with the use of adequate oxygen, their activity is limited due to dyspnea. For certain patients, the insertion of the transtracheal oxygen catheter, a catheter that delivers oxygen directly in the airways, improves their exercise tolerance and their quality of life. This is an outpatient procedure and patients usually go home on the same day. This procedure is only available at a few centers in the country.
Asthma therapy
A new procedure has been developed to help patients with severe asthma and persistent symptoms despite optimal medical therapy. Airway thermoplasty uses heat to treat the muscles of the airways. It may help patients reduce their symptoms and reduce or phase out certain medications. Airway thermoplasty treats the main cause of airway obstruction in asthma patients, and it is available in our center through our asthma clinic.
Patient information & resources about airway thermoplasty
Diagnostic bronchoscopy
Electromagnetic navigational bronchoscopy enables the pulmonologist to reach areas in the lung using a special magnetic field. It enables the pulmonologist to biopsy very small nodules that previously required a CT-guided biopsy.
In addition to these procedures, our Interventional Pulmonology Program accepts referrals for all forms of diagnostic bronchoscopy and bronchoscopic lung biopsies.